| Gastroenterology Research, ISSN 1918-2805 print, 1918-2813 online, Open Access |
| Article copyright, the authors; Journal compilation copyright, Gastroenterol Res and Elmer Press Inc |
| Journal website http://www.gastrores.org |
Original Article
Volume 11, Number 5, October 2018, pages 346-348
Risk Factors of Cholelithiasis Unrelated to Hematological Disorders in Pediatric Patients Undergoing Cholecystectomy
Carmine Novielloa, c, Alfonso Papparellab, Mercedes Romanoa, Giovanni Cobellisa
aPediatric Surgery Unit, Salesi Children Academic Hospital, Ancona, Italy
bPediatric Surgery, Department of Women, Children, General, and Specialist Surgery, Campania University “Luigi Vanvitelli”, Napoli, Italy
cCorresponding Author: Noviello Carmine, Pediatric Surgery Unit, Salesi Hospital for Children, Via Corridoni, 11, 60100 Ancona, Italy
Manuscript submitted June 13, 2018, accepted July 2, 2018
Short title: Pediatric Cholecystectomy for Cholelithiasis
doi: https://doi.org/10.14740/gr1058w
| Abstract | ▴Top |
Background: Pediatric cholelithiasis unrelated to hematological disorders is an increasing disease. We analyzed our experience in the surgical treatment of these cases to evaluate risk factors, clinical presentation, intervention and follow-up.
Methods: From January 2010 to December 2016, we retrospectively recorded all data (hematological study, familiarity, use of lithogenic drugs and parenteral nutrition) of cholecystectomies for cholelithiasis not related to hematological diseases. The body mass index (BMI) was calculated (obesity if > 25), medical treatment, surgery and follow-up were evaluated. All patients underwent ultrasound for diagnosis and major biliary tract assessment prior to surgery. All patients had a 1-year follow-up.
Results: There were twenty-four cases (eight males), with a median age of 11.2 years. Predisposing factors were familiarity in 19, use of lithogenic drugs in 5 and total parental nutrition (TPN) in 3. Median BMI was 19.8 kg/m2, with BMI > 25 kg/m2 in eight cases. Regarding the clinical presentation, 14 had acute pain in the right upper quadrant, 5 had cholecystitis and 5 had non-specific abdominal pain. The medical treatment lasted 6 months in all, except for five (three operated after 2 months and two after 12 months). Preoperative ultrasound did not show stones in the biliary tract. MRI was performed in three cases for suspected malformation of the biliary tract (negative). Laparoscopic cholecystectomy was performed in all cases: mean intervention time was 95 min. A case of postcolecystectomy syndrome was found. At follow-up, all were asymptomatic, except two (recurrent abdominal pain).
Conclusion: Main predisposing factors are familiarity and obesity. Preoperative ultrasound in our series replaced the intraoperative study of the biliary tract. Laparoscopic cholecystectomy is the gold standard.
Keywords: Cholelithiasis; Cholecistectomy; Children
| Introduction | ▴Top |
Pediatric cholelithiasis is a relatively rare disease, but it is recently increasing [1, 2]. Ultrasound has become crucial in patients with abdominal pain, so today it is easier to diagnose pediatric cholelithiasis [3]. Laparoscopic cholecystectomy (LC) is a standard procedure for cholelithiasis not only in adults but also in children [4]. Indication to surgery is the symptomatic cholelithiasis without improvement after medical treatment. Several predisposing factors are reported, among them the hemolytic disorders are the main ones, although currently other conditions, such as obesity, create problems of the gallbladder that requires surgery. The authors report their experience in these patients by analyzing all the data of the children who had surgical treatment of cholelithiasis unrelated to hemolytic diseases.
| Patients and Methods | ▴Top |
Over a period of 7 years, from January 2010 to December 2016, the patients’ characteristics, operation procedures and outcomes of children with cholelithiasis, unrelated to hematological diseases, who underwent LC, are recorded. An informed consent was obtained for every patient presenting with biliary pathology. All patients in this study have undergone abdominal ultrasound, medical and medication history inquiry (to evaluate the use of lithogenic drugs or parental nutrition) and specialized assessment to rule out hematological problems. Body mass index (BMI) was calculated and considered for obesity if greater than 25 kg/m2. In each case of first diagnosis of cholelithiasis, medical treatment with ursodeoxycholic acid started at a dose of 10 mg/kg twice a day for at least 6 months. Except for five patients, after therapy, an ultrasound was repeated to check for calculi. Some cases underwent MRI to study the biliary tract. Those with symptoms despite the medical treatment have undergone LC. All patients underwent ultrasound examination the day before surgery to exclude stones of the main biliary tract (Fig. 1). The surgical procedure included an open trans-umbilical access, two operative trocars and an accessory trocar, the cystic artery and the cystic duct linked with the aid of metal clips. A low-fat diet has been recommended to every patient who followed a 1-year follow-up with clinical and ultrasound checks after 6 and 12 months.
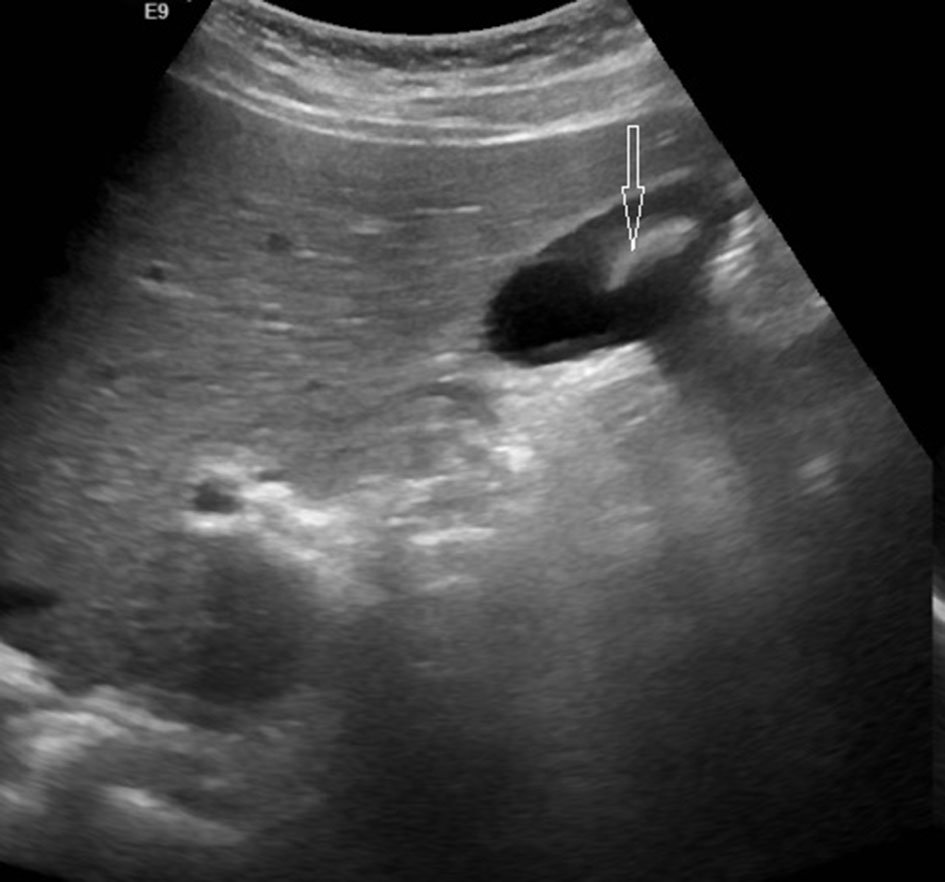 Click for large image | Figure 1. Ultrasound shows a big stone in the lumen of the gallbladder. |
| Results | ▴Top |
In this period, 24 patients (8 males) underwent LC. The mean age at operation was 11.2 years (range: 3.2 - 14.6 years). By analyzing the predisposing factors, we observed a familiarity with cholelithiasis (defined as parents affected by cholelithiasis in this study) in 19 children, use of lithogenic drugs (ceftriaxone or rifampicin) in 5 and total parental nutrition (TPN) in 3. Mean BMI was 19.8 kg/m2 (range: 11.8 - 37.0 kg/m2), with BMI > 25 kg/m2 in eight patients (33.3%). Regarding the clinical presentation, 14 children had abdominal pain at the right upper quadrant, 5 cholecystitis (abdominal pain, vomit and fever) and 5 cases with non-specific abdominal pain (Table 1). Medical treatment continued for 6 months in all cases but three, who underwent surgery after 2 months because of recurrence of cholecystitis, and two cases underwent medical treatment for 12 months (young patients). Preoperative ultrasound did not show stones in the main biliary tract in any case. MRI, performed in three cases due to biliary malformations, which were suspected at the ultrasound study, was negative. Cholecystectomy was performed laparoscopically in all cases; the mean time of surgery was 95 min (range: 50 - 155 min). A case of postcolecystectomy syndrome with nausea and diarrhea was treated medically (antispasmodics and ursodeoxycholic acid) for 1 month. At the follow-up, all patients were asymptomatic except for two who still complained of non-specific abdominal pain.
 Click to view | Table 1. Preoperative Data of the Patients |
| Discussion | ▴Top |
From 1722, when the first case of cholelithiasis was reported in an autopsy done to a 12-year-old boy, this problem has increasingly interested pediatric surgeons [5, 6]. The biliary lithiasis has a multifactorial genesis, with a large family component, characterized by alteration of cholesterol homeostasis and metabolism of the salts contained in the bile that precipitate forming the calculations. Cholelithiasis is often linked to hemolytic diseases that alter the solubility of bile salts, but today the form is not only increasing due to hematological diseases, but also due to the growing problem of pediatric obesity and use of particular drugs [6, 7]. In the series, the authors took into consideration the cholecystectomies performed in patients with cholelithiasis unrelated to hemolytic diseases in order to analyze the predisposing factors and the results of the surgical treatment. It is quite evident that the two most important factors are familiarity and obesity as reported in the literature [2, 8]. The use of lithogenic drugs or parenteral nutrition is less important, although they are influential factors. A point of discussion we raised in our study is how to treat cholelithiasis of asymptomatic forms, as currently the use of ultrasound allows the diagnosis of an incidental cholelithiasis in patients who have non-specific abdominal pain of other nature. This probably happened in two of our patients in whom non-specific abdominal symptomatology remained even after cholecystectomy. In these cases, we consider the use of performing the intervention, if ultrasound does not show improvement after therapy, to avoid subsequent complications. In our series, nobody had an intraoperative study of the main biliary tract, since in all the preoperative ultrasound did not show calculi in the main biliary duct.
In conclusion, obesity and familiarity underlie the increasing number of cholelithiasis requiring surgical treatment. LC remains, even in children, the standard procedure for treating these patients. Further studies are necessaries to define the treatment of patients with incidental finding of cholelithiasis and non-specific abdominal pain.
| References | ▴Top |
- Mehta S, Lopez ME, Chumpitazi BP, Mazziotti MV, Brandt ML, Fishman DS. Clinical characteristics and risk factors for symptomatic pediatric gallbladder disease. Pediatrics. 2012;129(1):e82-88.
doi pubmed - Suh SG, Choi YS, Park KW, Lee SE. Pediatric cholecystectomy for symptomatic gallstones unrelated to hematologic disorder. Ann Hepatobiliary Pancreat Surg. 2016;20(4):187-190.
doi pubmed - Wesdorp I, Bosman D, de Graaff A, Aronson D, van der Blij F, Taminiau J. Clinical presentations and predisposing factors of cholelithiasis and sludge in children. J Pediatr Gastroenterol Nutr. 2000;31(4):411-417.
doi pubmed - Balaguer EJ, Price MR, Burd RS. National trends in the utilization of cholecystectomy in children. J Surg Res. 2006;134(1):68-73.
doi pubmed - Walker SK, Maki AC, Cannon RM, Foley DS, Wilson KM, Galganski LA, Wiesenauer CA, et al. Etiology and incidence of pediatric gallbladder disease. Surgery. 2013;154(4):927-931; discussion 931-923.
- Akhtar-Danesh GG, Doumouras AG, Bos C, Flageole H, Hong D. Factors associated with outcomes and costs after pediatric laparoscopic cholecystectomy. JAMA Surg. 2018;153(6):551-557.
doi pubmed - Stender S, Nordestgaard BG, Tybjaerg-Hansen A. Elevated body mass index as a causal risk factor for symptomatic gallstone disease: a Mendelian randomization study. Hepatology. 2013;58(6):2133-2141.
doi pubmed - Frybova B, Drabek J, Lochmannova J, Douda L, Hlava S, Zemkova D, Mixa V, et al. Cholelithiasis and choledocholithiasis in children; risk factors for development. PLoS One. 2018;13(5):e0196475.
doi pubmed
This article is distributed under the terms of the Creative Commons Attribution Non-Commercial 4.0 International License, which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
Gastroenterology Research is published by Elmer Press Inc.


